Who is at Risk of Developing Skin Cancer?
Skin cancer can occur in anyone, but there are some factors that can increase your risk of developing skin cancer. Skin cancer often occurs in people who are exposed to a high level of ultraviolet light. This comes from the sun, especially during the middle of the day, or artificial sources such as tanning beds or sunlamps.
Individuals with a higher risk of developing skin cancer include:
- People with fair skin and who freckle easily.
- Individuals with light-coloured hair and eyes.
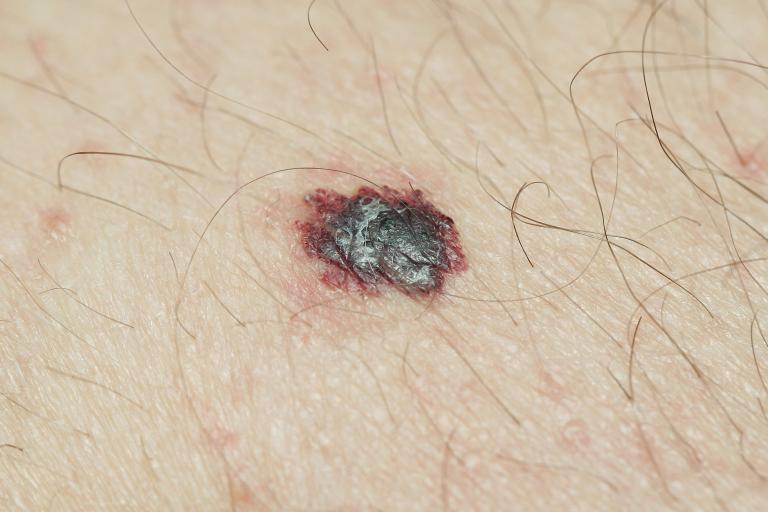
- People with a lot of moles, especially those that are abnormally shaped.
- Those with a family history of skin cancer or long history of blistering sunburn.
- People who work outdoors or spend a lot of time in the sun (particularly Squamous Cell Carcinomas).
- People who spend a lot of time in intense sunlight, like those who live closer to the equator or at high altitudes.
- Exposure to strong x-rays, radioactive substances (radium) or other chemicals such as coal tar, creosote or arsenic
- People with recurrent episodes of sun burn (particularly Basal Cell Carcinomas).
Skin is the Largest Organ in your Body- Take Care of It.
If you, your GP or your Dermatologist feel that you have a concerning skin lesion, we can check it and the rest of your skin to help detect and manage skin cancers early. We offer same day biopsy procedures if necessary and will discuss the options with you as to how best to manage the lesion. Where possible, we advocate for non-surgical management, including the use of medications or ointments to manage your skin lesions. We may take clinical photographs of the lesion for future comparison if we just need to keep an eye on the spot. If surgical excision is necessary, we will work with you to determine the best pathway to ensure a timely diagnosis and management. We will then continue to monitor your skin, as necessary, until a regular preventative regimen is established with your local doctor or skin check specialist.
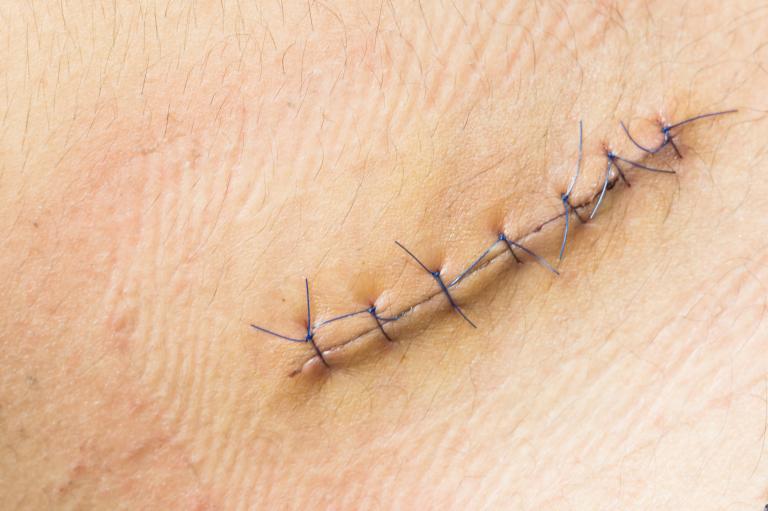
Do I need a Punch biopsy or an Excisional biopsy?
Punch biopsies involve taking a small, full-thickness sample of skin with a biopsy instrument that removes a short cylinder, or “apple core,” of tissue. After a local anaesthetic is administered, the instrument is rotated on the surface of the skin until it makes a small core, containing all the layers, including the dermis, epidermis, and the most superficial parts of the subcutis (fat).
When the entire tumour is removed, the procedure is called an excisional biopsy. When possible, excisional biopsy is the preferred method when melanoma is suspected so that the characterstics of the entire lesion can be used to determine what additional treatment (including skin margin and other diagnostic tests) is necessary.