What is a Mandibulectomy and Free-Flap Reconstruction
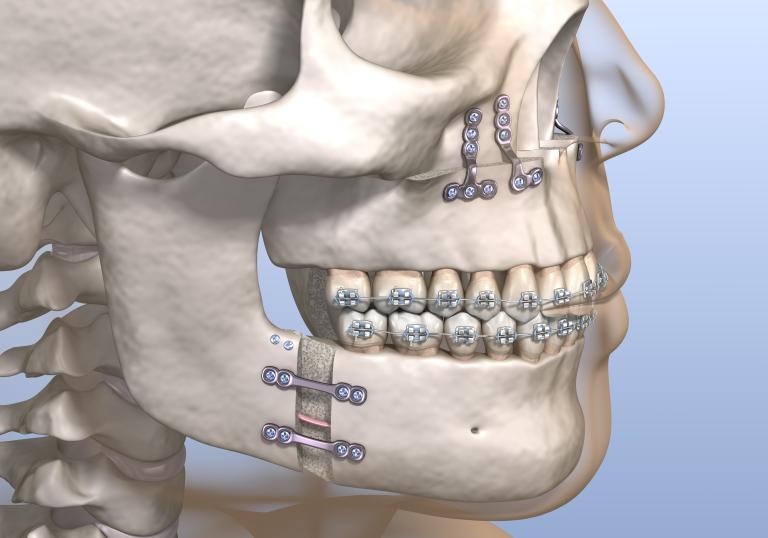
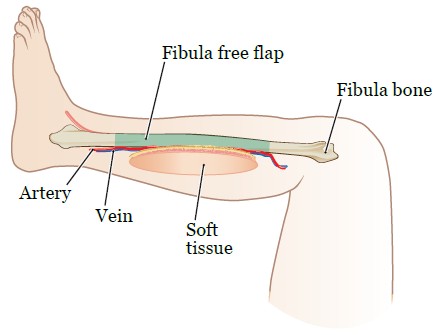
During a mandibulectomy your surgeon may use bone from your leg (fibula) to rebuild your jaw. When using a fibula free flap they will also remove an artery, vein and soft tissue along with the bone.
The donor site may also need a skin graft. This is done by taking the top layer of skin from another part of your body and moving it to the donor site that needs to be covered. The skin graft is often taken from the buttock or thigh, but your surgeon will discuss these details prior to your surgery.