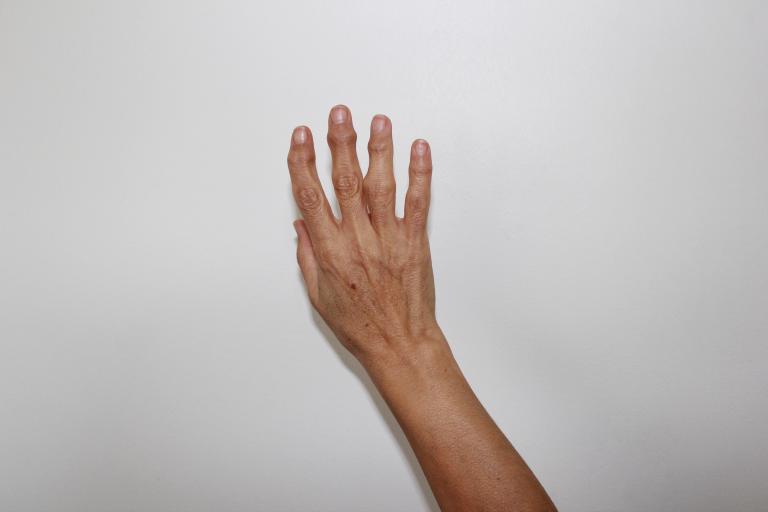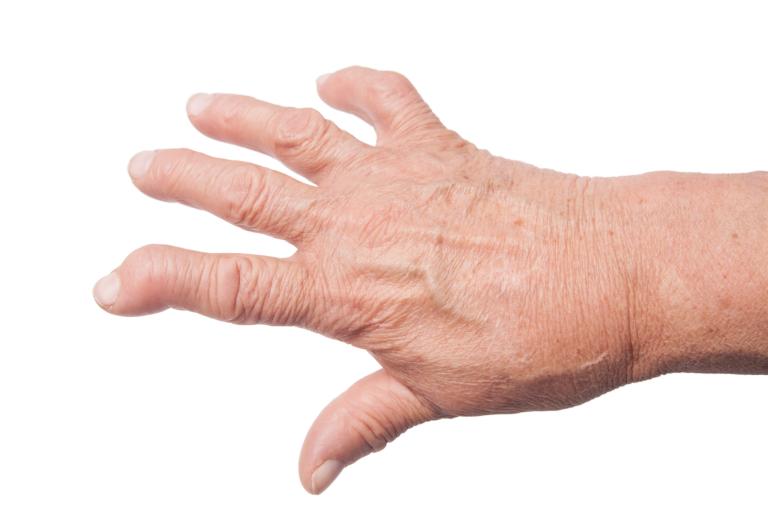
What types of surgery does my RPS surgeon do for arthritis?
- Arthrodesis: involves fusing (joining) the two bones forming the joint together. As the fused joint cannot be moved it is no longer painful. This type of surgery is most commonly done on ankles, wrists, fingers or thumbs.
- Resection: is the removal of part or all of a bone or an entire joint. This is often done for damaged joints in the foot and big toe.
- Synovectomy: is an operation to remove the lining of the joints, the synovium. This is effective for rheumatoid arthritis, to reduce pain, swelling and joint damage. However the synovium may regrow several years later and the symptoms can return.
- Joint replacement: is also called arthroplasty. This involves the removal of damaged surfaces of the joint. These surfaces are then replaced with metal, ceramic or plastic parts. The entire joint can be replaced (total arthroplasty) or just one part of the joint (hemiarthroplasty). Joint replacements can be done on knees, hips, shoulders, elbows, fingers, ankles, toes and even the spine.
All of these surgeries are best performed when non-operative management (including management by a specialist Rheumatologist for rheumatoid arthritis) and medications are already optimised and there is an agreed plan for surgery to help with specific issues within the hand as part of on-going non-operative management approaches.