How is Dupuytren’s Disease Treated?
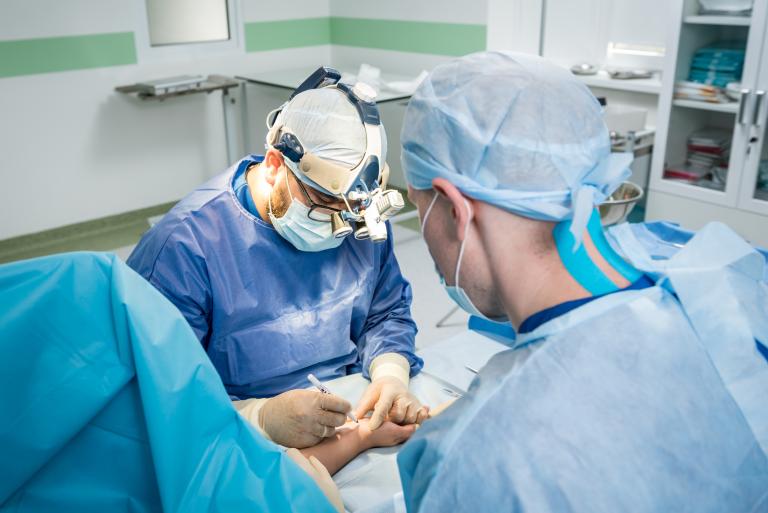
Surgical treatment of dupuytren’s disease
There are two main procedures to treat dupuytren’s disease- fasciectomy and needle fasciotomy.
In fasciectomy the diseased cords are surgical removed and the surgeon may also perform a joint release when a joint is immobilised in a flexed position. Fasciectomy is the most successful of treatments, however there is risk of recurrence of approximately 20% within 4 years.
For patients who will not tolerate a full fasciectomy, a limited fasciectomy will remove a small amount of the diseased tissue and correct the flexed finger deformity. While there’s a high recurrence rate with this surgery, it’s commonly performed on elderly patients who aim to improve hand function.
The second type of procedure is called needle fasciotomy. In this procedure, the hand is anaesthetised and then a needle is used to divide the fibres in the cord until the finger can be stretched to a straighter position. This is safest when performed in the palm (rather than the fingers) and while it does not remove the diseased cords, it stops them from pulling down on the affected fingers. This is generally well tolerated by most patients, including the elderly and those with pre-existing medical conditions. It can provide a good functional benefit, but has a higher rate of recurrence than fasciectomy.
Our RPS surgeons will conduct a thorough assessment and determine whether any of these approaches is right to manage your Dupuytrens disease.